Organizations providing health care are seeking to improve their patients’ experience while navigating increasing operational complexity. The increasing number of patients, fragmentation of systems, and significant regulatory constraints create challenges in delivering consistent personalized care at large scales. Many providers predict that by 2026, more traditional “management” and “general” CRM systems will be insufficient. Therefore, many organizations are choosing to implement purpose-built healthcare CRM systems that are developed in collaboration with an experienced healthcare software development company to ensure an understanding of the clinical workflow, compliance with patient privacy, and the long-term requirements of the system.
Healthcare CRM software offers more than just a method for collecting and storing patient contact information. It functions as a layer of coordination that connects the communications from all departments together with care workflows and operational data. This article will explore the design of today’s healthcare CRM systems, the problems that they solve, and important factors to consider when building or updating these systems.
What Makes Healthcare CRM Different From Traditional CRM
Conventional CRM applications handle lead and sales pipeline management and diagnosing customer relationships mainly within the commercial domain. But when considering the healthcare domain, healthcare CRMs attempt to meet the unique requirements of this ecosystem.
Healthcare CRMs should facilitate:
- Various roles of users within the healthcare ecosystem (patients, clinicians, administrators, care coordinators, and other support staff).
- Security of individuals’ health and personal information that is governed by regulation.
- Building of long-term patient relationships (rather than just working on transactions).
- Integrating with clinical, operational, and financial systems.
The primary focus of a healthcare CRM platform is continuous healthcare delivery, trust, and compliance, rather than being driven by sales. In addition to usability, healthcare delivery systems look for data integrity, access control, and audibility of activities.
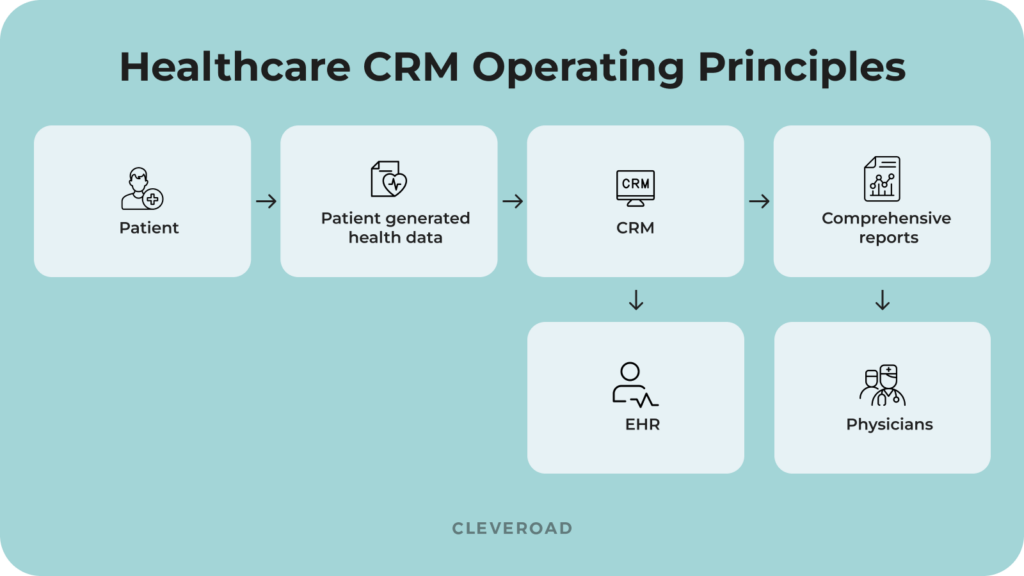
Core Problems Healthcare CRM Software Solves
Efficient care coordination is vital to delivering care. It requires collaboration between internal departments, specialists and external providers. The use of disconnected systems will lead to slowed coordination, duplicate task completion, missed follow-up appointments, causing delays in patient care and gaps in care delivery.
The use of a healthcare CRM provides centralized coordination of all activities related to the coordination of patient care, including the management of referrals, task management, scheduling of follow-ups, and structured communication amongst the healthcare team. The clear assignment of owners and shared timelines will increase the efficiency of the teams and provide for continuity of care during the patient’s journey through the healthcare system.
Success is now based on patient engagement, patient reverence, and patient satisfaction, not just visit counts like before. CRM analytics improve patient engagement, missed appointments, response times, and operational issues by providing actionable insights for hospitals to make data-driven improvements.
Core Components of a Modern Healthcare CRM
Patient Profiles and Identity Management
A healthcare CRM is based around complete profiles of patients that include more than basic demographic information. An example of this is:
- Contact and communication information
- Interaction logs and appointment history
- Follow-up activity, such as a care plan
Consent status and authorization status
The identity management function makes sure that access is provided according to a person’s role/responsibility or regulatory requirements.
Identity management ensures that access to communications, such as mail or SMS, is done according to the patient’s preferences and consent to receive those communications (not for promotional marketing purposes).
Notifications, such as reminders of appointments and follow-up messages
Educational content delivery
Tailoring communications to be relevant, timely and in accordance with each patient’s preferences for consent to receive such communications, rather than promotional communication purposes.
Workflow and Task Automation
The CRM supports managing internal processes for a business, including:
Assigning follow-up tasks
Coordinating referrals
Escalating the resolution of patient requests that have not yet been resolved
Tracking of care plan progress
Automating many of the administrative aspects of these tasks allows staff to reduce their time spent on administration while making responses to patient interactions consistently.
Integration With Existing Clinical and Operational Systems
Healthcare CRM systems, in general, are designed to work with instead of replacing existing systems. The most common means of integration include:
- EHR or electronic medical record systems
- Scheduling and appointment systems
- Billing and insurance record systems
- Telemedicine solutions
Integration helps to ensure that there is a common set of information across all systems and preserves the boundaries of the systems that control that information.
Analytics and Reporting
Healthcare CRM analytics are focused on:
- Tracking of patient engagement trends and communications
- Measuring the effectiveness of communications
- Managing the efficiency of coordinating care
Measuring the distribution of operational workload across the business, so the organization is able to identify any areas that may have a deficiency, and provide appropriate corrective actions
Healthcare CRM Use Cases by Provider Type
Digital health providers rely on CRM platforms to facilitate patient journeys through all stages of care, including onboarding, scheduling, virtual consultation, and post-consultation communication. Centralizing the management of these activities creates a consistent and continuous relationship between the patient and provider/delivery system during asynchronous and remote interactions.
Home health and chronic care providers utilize a CRM system to track patient interactions with multiple caregivers during their ongoing care and to monitor patient adherence. This systematic approach of managing patients ensures continuity of care over a long period of time and provides an opportunity for continued access and visibility during a complete patient journey.
Security and Compliance Requirements
When developing a healthcare CRM patient management system, it is important to design it with security and compliance as one of its first priorities because they are both important to protecting sensitive information from unauthorized access or use, as well as meeting all applicable privacy laws.
Developers will want to consider these five aspects of the system during their design phase in order to avoid expensive changes later.
- Data must be encrypted when stored and transmitted through an application (e.g., via email).
- Users should only have access to data that they need in order to perform their job based on their assigned role. (e.g., A clinician will only have access to patient records they are treating.).
- A log should be maintained of any activity that occurs to or touches the patient, and it should be possible to find this log of activities for each patient.
- The system should support both obtaining patient consent to collect, use and disclose their personal health information and maintaining the history of the use of that information.
- Prior to the start of the design of the system, a process must be developed to evaluate third-party products being considered to integrate with the patient management system.
When the beginning of a project does not give consideration to these points, the end of the project will probably be a significantly more expensive redesign of the system.
Architecture Considerations for Scalable Healthcare CRM Systems
Designing A Modular System
A modular design for a healthcare CRM allows an organization to increase in size and adapt functionality without interfering with any previously established aspects of that system as it grows. Modular systems architecture separates out key individual components of the system (e.g., patient records, communication capabilities, analytics capabilities, and integration tools) into multiple independent modules, which allows the addition of new capabilities, modifications to the existing workflow(s), or a complete replacement of a key module without having a negative impact on other previously established capabilities.
The ability to remain flexible is particularly important for healthcare organizations that need to respond to frequent changes to regulatory requirements, new models of care delivery, and variations in how care is provided. Modularly designed systems also have decreased development risks because implementing changes will have a limited impact on other existing capabilities and will generally be easier to test. The development team can incrementally implement changes to the system (as opposed to performing “large” or “all at once” changes) and validate changes to modules independently without the risk of significant regression across the entire network.
Cloud-Native Infrastructure
The cloud-native infrastructure is critical to delivering the scalability and reliability necessary to support modern healthcare CRM systems. Deploying a cloud-based platform allows organizations to manage fluctuating workloads (e.g., long peaks in demand associated with scheduling appointments, significant spikes in communication activity) without impacting the performance and reliability of their application environment. High availability and redundancy provided by a cloud environment significantly decrease the risk of downtime for an organization’s user community, which is critically important within the healthcare industry. A cloud-native infrastructure also simplifies the IT organization and is accomplished through the automation of update processes, monitoring processes, and backup procedures. Furthermore, using a cloud-native infrastructure allows for greater predictability relative to operational expenditures, as cloud resources can be scaled to meet actual demand. Additionally, disaster recovery and maintaining data resiliency are also significantly simplified within a cloud environment, allowing for the continued delivery of service to customer organizations.
.
API-First Integration Strategy
An API-first integration strategy ensures healthcare CRM platforms connect reliably with various external systems. CRMs must exchange data with EHRs, scheduling tools, billing platforms, telemedicine systems, and analytics services. Well-defined APIs create clear system boundaries, reduce tight coupling, and simplify maintenance. This approach allows organizations to add or replace integrations without redesigning the core CRM. improves data consistency and security by enforcing standardized access patterns and validation rules. Over time, this flexibility helps healthcare organizations adapt to new technologies and partners while preserving system stability.
Final Thoughts
Developing CRM software for the healthcare industry requires a focused approach that adheres to clinical practices and workflows, adheres to laws, regulations, and patient needs, etc. The benefit of investing in an effective CRM system is much more than just having an efficient operation; it will also enhance your relationship with patients, improve the coordination of your teams, and create an expandable platform for the delivery of digital healthcare.
As part of a connected health system, a CRM will act as the key layer to link data, communication, and care together to form one complete solution.
Author’s bio

Yuliya Melnik is a technical writer at Cleveroad, a web and mobile application development company specializing in healthcare software solutions. She writes about digital health, patient-centric technologies, and software systems that support better clinical outcomes and everyday medical workflows.
